I was interviewed by Rob Schware and this interview was posted on Huffington Post yesterday. That is really awesome. I feel proud and happy seeing the end result.
Please read the interview down here or at the place of origin by clicking here.
 This is an interview with Anneke Sips, a yoga teacher and social psychiatric nurse (RN) from Amsterdam, the Netherlands. For the last 16 years she has been working in the field of psychiatry; she started teaching yoga eight years ago. She studies with TKV Desikachar’s son and the Mohan family — both in the tradition of Krishnamacharya .
This is an interview with Anneke Sips, a yoga teacher and social psychiatric nurse (RN) from Amsterdam, the Netherlands. For the last 16 years she has been working in the field of psychiatry; she started teaching yoga eight years ago. She studies with TKV Desikachar’s son and the Mohan family — both in the tradition of Krishnamacharya .
Rob: What originally motivated you to do this work, and what continues to motivate you?
My own experience is the best motivation for me. Yoga always helped me through the waves of life. Since I found yoga, my dream was to connect my passions (yoga and psychiatry). However, I wasn’t sure how, and I wasn’t verbally strong enough to convince the psychiatrist of the ward where I worked then, who was against the idea. I couldn’t get this out of my head. Then, early in 2010, I decided to go to Rwanda with Project Air to teach yoga to traumatized people with HIV. I volunteered for three months. After all I saw there, I was more motived than ever to bring yoga into my work. Knowing the challenges in bringing this mind-body approach into a medically-oriented space, I felt the need to study more, and to find people to build community. I started a network on LinkedIn, and in 2010 I organized the first Yoga & Mental Health Sangha for all who are interested in the field of yoga and mental health in Amsterdam. Since then, twice a year we meet with the community to talk, share, inspire, and connect. May 2014 is the next Sangha in Amsterdam.
 Is there a standout moment from your work in Rwanda?
Is there a standout moment from your work in Rwanda?
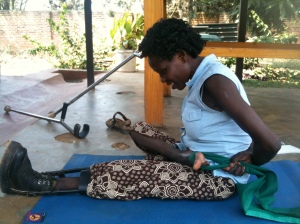
When I was teaching there for Project Air, there wasn’t a beautiful yoga studio to be found. The people didn’t know about yoga before Project Air came. They had no preconceptions. They just practiced and it felt good! One experience: I taught in an empty, dusty little church on a hill. Once, we were locked out of the church, so we sat on the yoga mats under a tree in front of that church while I told them about the origins and philosophy of yoga. Then I asked for their experiences. One by one they began to talk about what yoga does for them. They said that they were able to sleep through the night since the genocide in ’94, now that they practice yoga. “I feel my body again,” said another, squeezing her own hands and arms. “I have less trouble with the side effects of my HIV medications.” “I feel happier.” The stories went on and on and they recognized each other’s experiences. When I think back to this afternoon under that tree, I still get tears of joy in my eyes: the true nectar of yoga!
What did you know about the population you are working with before you began teaching?
I am experienced in working with people who have chronic psychiatric illnesses. Most of my patients suffer from a psychotic disorder, in combination with drug abuse and trauma. But also we see many stress- and anxiety-related issues, depression, and personality disorders.
What are two distinct ways that your teaching style differs from the way you might teach in a studio?
In a trauma-sensitive class, or working with any population in mental health care, I would not — or rarely — touch somebody or give physical adjustments. I don’t want to trigger them and make the yoga session unsafe. This made me re-think my touching in a regular class too. Also, in my experience, teaching special populations requires a more personal approach than general teaching in a studio.
How has this work changed your definition of yoga and your practice? Your definition of service?
As I said, when teaching special populations, I create a more personal approach by teaching them one-on-one or in small groups. I think this personal approach is important, also in a regular class. Everyone is different and yoga has so many great tools that can assist every person in any challenge or at any stage of life. In my studies and practices I am diving deeper into the philosophy of yoga; yoga is a part of my life, rather than an asana practice on my mat. I feel like unraveling my practice into the unknown, off the mat; it’s a place where stillness appears, and growth and transformation are possible.
Since I use yoga in my work, I observe people and have become a better listener as a nurse, too. I have become more mindful, and see the self-healing qualities in my patients better. It helps me to “sit in my hands” more, which empowers the patients, help them trust their body signals and intuition again. It’s de-stigmatizing to support them to help themselves. What society sometimes thinks of as the “weak ones” I see as the strong ones — survivors in tough circumstances.
What has been the greatest challenge in your teaching experience, and what tools have you developed for addressing these? What advice would you give to anyone who is going to teach in the population you work with?
A great challenge is bringing yoga as a therapy (not just an activity) in a medical setting. I approach this professionally, but follow my intuition and heart. I advise to “walk the talk” and use good research on yoga. Set up a plan and evaluate. Study, practice, and research gave me the confidence to start the discussion. The community is helpful here for reflection.
Self study and practice, experience, right intentions, observation, and compassion are needed to grow as a teacher/therapist. I think whoever wants to teach specific populations should learn about them. I believe yoga is a safe practice to teach, if you know what you are doing, and have the skills to avoid triggering trauma.
What are some of your hopes for the future of “service yoga” in the next decade?
I hope that yoga becomes an evidence-based practice that will show up in the guidelines of treating mental illness. I hope that yoga teachers and therapists stay true to the yoga teachings, and keep the Yamas and Niyamas in mind, so that practices result in peace of mind.
Editor: Alice Trembour
Images: Courtesy of Delight Yoga Amsterdam and Anneke Sips